Optimize Pricing and Billing for Medicare Plans
Growth of Medicare Advantage plans in the U.S
The healthcare market is witnessing robust growth. Enrollment in the Medicare Advantage (MA) program has more than doubled over the past decade fueled by an aging population. By 2030, more than 20% of the U.S population will be over the age of 65. With an aging population in the US, nearly four in ten (39%) of all Medicare beneficiaries or 24.1 million people out of 62.0 million Medicare beneficiaries overall are enrolled in MA plans. Between 2019 and 2020, total MA enrollments grew by approximately 2.1 million beneficiaries or 9 percent. Moreover, enrollment in Medicare and Medicare Advantage plans has been snowballing over the past several years as consumers seek reduced costs and improved outcomes. And, COVID-19 has accelerated interest—45% of original Medicare enrollees are switching to a MA plan for 2021.
A Deep Dive Into Medicare: Optimizing Pricing and Billing for Medicare Plans
While the growing interest in MA plans presents a unique opportunity, many healthcare payers are relying on legacy systems that are not designed to deliver the agility, flexibility, and insight that today’s MA plans require. Additionally, as payers seek to optimize billing reconciliation and make better use of their data, they must first address their growing pain points. Find out how to address these issues with Oracle's enterprise-wide revenue management and billing solution that helps healthcare payers deliver transparent billing and provide a better member experience.
Member satisfaction is essential according to CMS
According to J.D. Power’s 2020 Medicare Advantage Study, only 15% of MA plans meet key performance indicators that help drive satisfaction and trust with members, which are drivers of the CMS (Centers for Medicare and Medicaid Services) advocated Medicare STAR ratings program. Moreover, members want a better experience as they are choosing 4+ star rated MA plans.
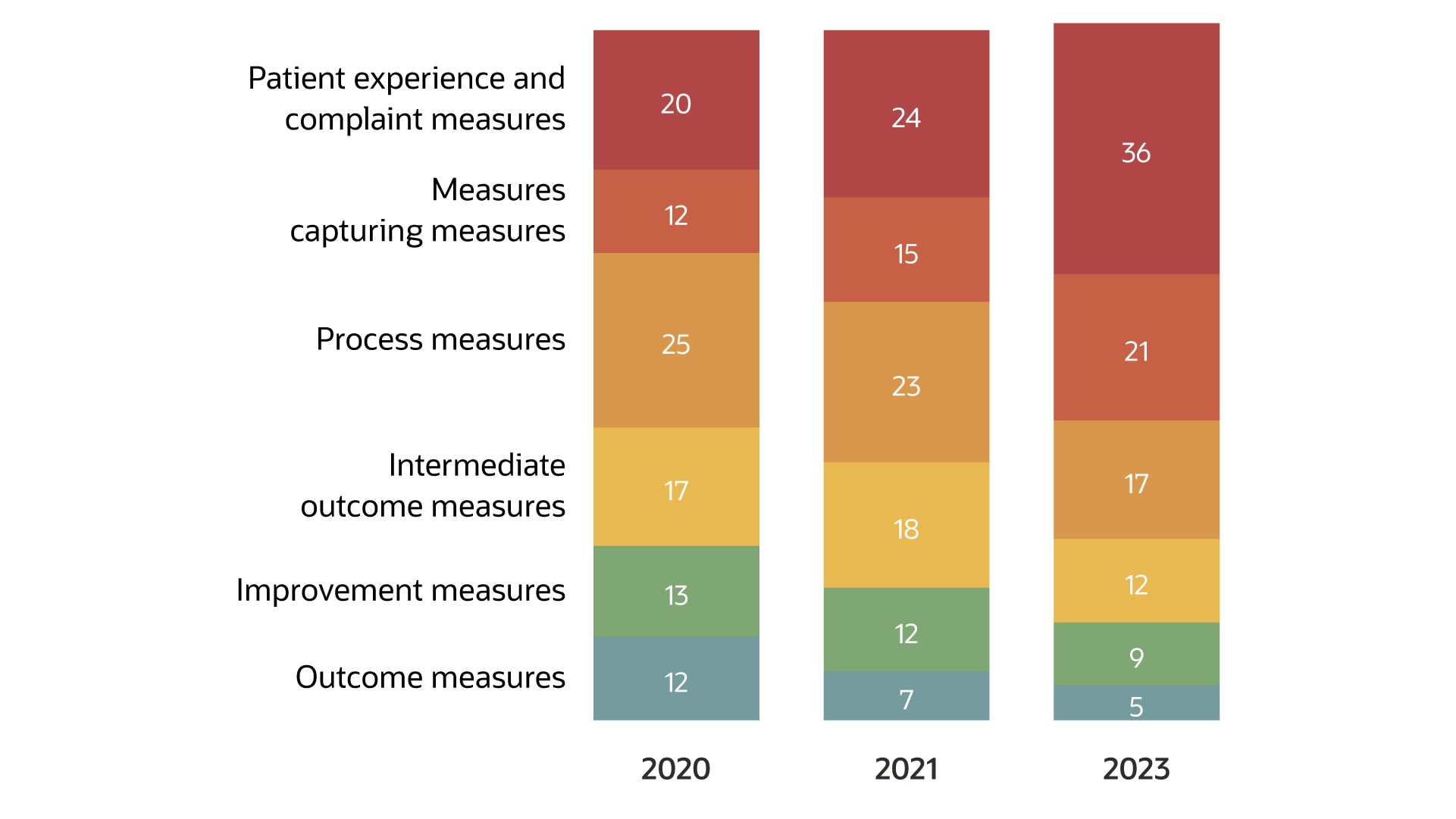
What do members want?
Members want accurate discounts on their billing, not just digital initiatives. Premium pricing and billing are key member touchpoints that have the potential to offer a differentiated consumer experience. Members may not care much about a health plan’s digital initiative like an attractive website or a multifunctional mobile app if the bills they receive are not timely or inaccurate. They may prefer not to spend hours on the phone with a call center representative, seeking clarification on a subsidy amount from the government that was not posted on their previous bill. Medicare Advantage plans cannot risk such experiences with their members that could decrease the overall satisfaction scores.
A big step forward to solve these problems is deploying a unified pricing and billing platform that helps improve the member experience.
“A big benefit in consolidating down to one single billing system was the ability to report internally and externally, so we are able to track delinquency, unbilled and all other types of metrics to show we are billing timely and accurately.”
Operational challenges and desired state
| Operational challenges that healthcare payers face with Medicare and Medicaid plans | Desired state |
|---|---|
| Increasing administrative costs for government plans—maintenance of multiple legacy systems and support processes | A single pricing and billing platform that supports all lines of business for payers and sponsored government plans |
| Data mismatches between healthcare payers and CMS enrollment records | Seamless data exchanges between multiple systems, payer’s enrollment platforms, and CMS Medicare record system to ensure there are no differences |
| Lack of real-time data sharing, delays due to retroactivities, manual processes, and payment discrepancies between CMS and payers | Automated billing reconciliation and dispute management system coupled with a single dashboard to view, track and drill down on specific payment and discrepancy |
| Vast variation across states and counties to manage Medicaid plans | Flexible platform that is largely driven by configurations over coding for Medicare and Medicaid plans |
| Meeting member expectations for empowerment and transparency and CMS rating requirements | A modernized billing system that enables payers to meet the expectations of a new generation in terms of multiple plan offerings, accurate and transparent billing, and enabling real-time payment anytime from any device, etc. |
Oracle's approach: Revenue management and billing for Medicare and Medicaid plans
Oracle has designed a Member 360 view that enables access to all billing information, including member hierarchy, pricing rules, bill and payment history, and member contact timelines. We aim to deliver a complete solution for healthcare payers with the capability to drill down to the individual bill line level for Medicare Advantage plans.
A comprehensive premium calculation, billing, accounts receivable, and collections solution that offer end-to-end capabilities for government plans
Member 360
Complete, cross-product, Member 360 dashboard to view Medicare and Medicaid billing statements and payments
Payment Reconciliation
Automated reconciliation framework for matching CMS payments and Social Security Administration (SSA)/Railroad Retirement Board (RRB) withholds
Configurable Pricing and Billing
A single solution for Medicare group and individual billing, retroactive billing and flexible rules for state Medicaid plans
Financial Accounting
Integrated sub-ledger with deferred revenue recognition for government plans
Oracle Revenue Management and Billing—platform of choice for leading healthcare payers
At one of the largest U.S based payers, five legacy billing systems across various lines of business were consolidated onto Oracle Revenue Management Billing (ORMB), reducing the overall infrastructure support costs by approximately 50% while improving efficiency, simplifying operations, and elevating customer experience.
Understand how Oracle Insurance Revenue Management and Billing can help you to optimize pricing and billing for Medicare plans.