Oracle Health Insurance: Modernizing Claims Processing and Adjudication
When it comes to claims management, few areas of the healthcare lifecycle deliver greater opportunity and risk. It is a critical area where relationships are sealed or severed, and business performance is strengthened or forfeited. Health insurers understand the importance of claims management and adjudication, and how it desperately needs innovation. Let's survey the healthcare landscape and make a plan for happier customers and stronger business performance.
Claims as Key to Customer Experience
In 2019, health insurance companies ranked near the bottom of the American Customer Satisfaction Index, on par with airlines and just below wireless telephone service providers. Numerous factors contribute to this standing, and claims is an important player. In looking at specific customer satisfaction benchmarks for health insurance providers, satisfaction with timeliness of claims payment is at the bottom of the list, followed only by call center experience satisfaction.
In Australia, customer satisfaction of private insurance fluctuates—with a rating of 72.2% in August 2019 after reaching its lowest rating of 70.5% in June 2018. As a result, Australian enrollment in private health insurance is declining. According to the latest Australian Prudential Regulation Authority (APRA) figures, private hospital treatment memberships fell by 30,174 in June 2020—a decline from 44.3% of population in June 2019 to 43.6% in June 2020.
At the same time, plan sponsors and consumers are paying more than ever for premiums and out-of-pocket costs. In the U.S., The Kaiser Family Foundation’s 2019 Employer Health Benefits Survey found that average annual family premiums for employer-sponsored health insurance rose 5% in the past year to $20,576. Consider, too, that the average premium for family coverage has increased 22% over the last five years and 54% over the last ten years, significantly more than either workers’ wages or inflation. Employees are paying more as well. The average dollar contribution for family coverage has increased 25% since 2014 and 71% since 2009.
Plan members and sponsors want more for their dollar, including a better claims experience
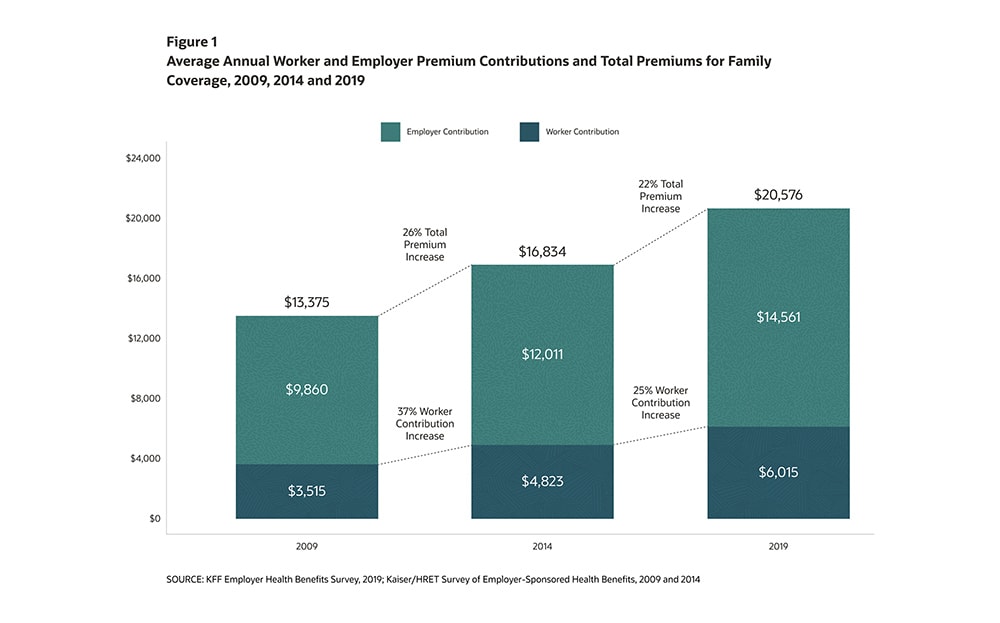
Figure 1 Average Annual Worker and Employer Premium Contibutions and Total Premiums for Family Coverage, 2009, 2014 and 2019
SOURCE: KFF Employer Health Benefits Survey, 2019: Kaiser/HRET Survey of Employer-Sponsored Health Benefits, 2009 and 2014
High Cost of Claims Processing—For Health Insurers and Providers
Claims processing is an expensive proposition for both health insurers and participating providers. Let’s consider the impact:
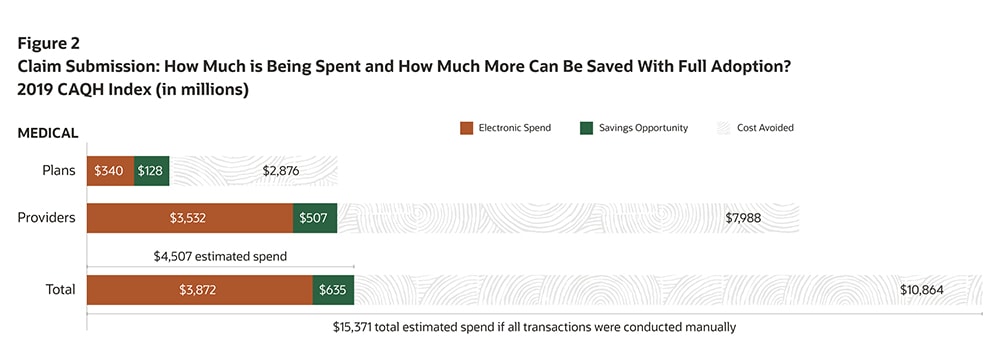
Figure 2 Claim Submission: How Much is Being Spent and How Much More Can Be Saved With Full Adoption? 2019 CAQH Index ()in millions
$15,371 total estimated spend if all transactions were coducted manually
- The medical industry in the U.S. spends $4.5 billion annually (PDF) on claim submissions, representing 13% of the total medical industry spend on administrative transactions.
- Australia reported a deterioration of insurance performance in June 2020 as a result of lower premium revenue, higher claims, and higher management expenses. Management expenses alone increased by 15.8% to $650 million in June 2020.
- The medical industry—providers and health plans—could save an additional $454 million annually (PDF) by transitioning to fully electronic transactions—$355 million for providers and $99 million for plans.
- Claim status inquiry was the second most expensive transaction (PDF) to conduct manually ($10.13) and electronically ($2.41) for the medical industry. The medical industry could save over 42% of the existing spend on claim status inquiries (PDF), or $2.2 billion, by moving manual and partially electronic web portal inquiries to fully electronic transactions. The savings potential associated with claim status inquiry is the second highest savings opportunity for the medical industry behind eligibility and benefit verification.
Time to Digitize Claims Processing
The increased cost and complexity of claims processing and adjudication presents both an urgent challenge and unique opportunity for health insurers. In many countries (PDF), insightful claims analytics remains a challenge. With restrictions on data available from insurers and the lack of consistency in diagnosis coding, the burden falls on the policy holder to access better claims data.
Digitizing claims processing and adjudication can streamline operations, increase accuracy, and boost efficiency—and ultimately provide a better customer experience. Even moving to a partial digital model can help transform claims management. Payors can save as much as 10-20% of medical costs by turning to a digital solution and reduce operating expenses for claims processing by up to 30%.
When selecting technology to support a claims modernization initiative, health insurers should focus on four critical capabilities:
Flexible product definitions:
Insurers should look for a solution that offers tiered categorization of health services and separates benefit specification from the cost-sharing model—driving maximum configuration reusability. In addition, it is important to have the flexibility to define benefits in a wide range of code sets and store parameter definitions separate from parameter values to simplify changes during renewals.
Agile claims pricing:
Today’s health insurers need to support a wide range of pricing methods, so they require extensive business rule-types for pricing calculations. Insurers should seek a solution that offers template-driven setup of provider contracts and pricing clauses, automates support for pricing claims, and enables provider payment amount per claim line, per admission, and per diagnosis. A solution should also calculate retrospective or prospective bundled payments across multiple claims and multiple procedure reductions within a single claim and across multiple claims.
Real-time claims adjudication:
This capability is a high priority for insurers and one that can offer considerable savings while elevating service. It starts with the ability to automate bundling of claims into a single episode of care. Insurers should seek a solution that offers pre-configured process flow and the ability to achieve high auto-adjudication rates through flexible benefit selection, iterative authorization matching, duplicate claim recognition, automated filing limit detection, and external callouts. In addition, insurers require configurable claims messages, the ability for mass reprocessing, and integration of benefit accumulation and external providers. To ensure control, insurers also require the ability to place global financial holds on payment transaction.
Automated authorization:
This capability goes hand-in-hand with real-time adjudication. Health insurers seek full authorization and referral management capabilities that enable authorization from multiple case and clinical management systems and support unlimited service lines per authorization. While insurers seek automation, they also need the flexibility to grant key one-off authorizations directly into the system. In addition, a claims modernization solution should offer the ability to capture extended data and attachments with the authorization request and enable fully configurable preauthorization matching rules.
Winning in a New Era—Customer Success Stories
Meet two health insurance innovators focused on the benefits of claims modernization with Oracle Health Insurance:
Liberty Health:
Liberty Health saw its business changing as customers seek greater transparency, personalization, and convenience. However, the company’s legacy infrastructure wasn’t equipped to propel it into the future of digital information and healthcare.
Liberty Health selected Oracle Health Insurance as the vehicle for its transformation journey. The organization is focusing first on automation and improving process efficiency as a foundation for a better member experience. Business processes that used to take two to three days now take just seconds.
Learn more about Oracle's Health Insurance Solutions