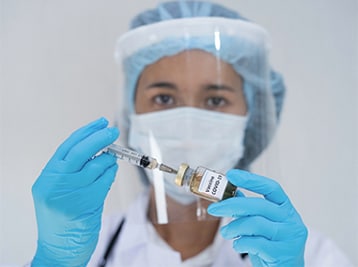
This vaccine-safety app built for COVID-19 offers a model for people-friendly health data collection
Dreams of getting real-time data in healthcare are becoming a reality—driven by changes caused by the COVID-19 pandemic.
By Margaret Lindquist | May 2021
In March of 2020, more than 50% of the clinical trials running at the time were shut down, for two main reasons.
One, pharmaceutical companies and researchers turned their attention to treatments and vaccines for COVID-19. And two, those that tried to keep running needed to figure out how to operate when patients couldn’t come into offices or health centers for their trial visits.
Clinical trial operators needed new, decentralized data collection models, tapping into telemedicine, digitized source data (eSource), and electronic consent forms (eConsent).
Those new techniques are likely to stick well past the pandemic.
“Researchers had to pause and think, and they've come up with new ways to conduct clinical development,” says Katherine Vandebelt, global vice president of innovation for Oracle Health Sciences. “Since the pandemic didn't just last for three months, they're starting to realize that not only was this a mitigation strategy, that this is actually a better way of doing the work.”
“The focus going forward will be on data quality, risk management, making sure that the data being collected is correct and proper and fit for purpose for how it’s going to be used.”
The biggest examples of this revolution in health science and data collection come directly from COVID-19, with the massive effort to collect real-world data to monitor the safety and efficacy of the vaccines that the scientific community so quickly created, tested, and brought to market. A mobile solution called v-safe sits at the heart of that effort in the United States.
A new kind of health tracker
The v-safe after vaccination health checker was created by Oracle developers for the US Centers for Disease Control and Prevention (CDC), using the Oracle APEX low-code development tool, Oracle Analytics, and Oracle Cloud Infrastructure. People who receive a COVID-19 vaccination can register with v-safe to voluntarily report side effects, such as pain or nausea, for the first days, weeks, and months after injection. The CDC can reach out to people who have experienced a concerning adverse reaction to gather more data, and medical professionals use this data to better understand how different patients and populations—particularly at-risk populations—respond to different vaccines.
Most recently, the New England Journal of Medicine released a study using data collected by v-safe that offered reassuring news about the safety of vaccines on pregnant women. “One of the CDC’s responsibilities is to gather as much information as they can about a population,” says Vandebelt. “For example, clinical trials with pregnant women had not been conducted, so the real-world data provided insights that the clinical trials did not.”
According to CDC officials, v-safe represents active, timely scrutiny of COVID-19 vaccines, rather than the passive surveillance of older systems that required patients or healthcare providers to go to a web site and submit a lengthy report online or fill out a paper form. The key difference is that once a recipient registers for v-safe, the registrants will receive quick and simple check in requests, so recipients don’t need to remember to report or decide that a symptom isn’t serious enough to report. Once a recipient registers on their smart phone, they’ll receive a text message every day for first week after first dose, a second dose reminder, a text message every week after the vaccination is complete and then reminders at months three, six and twelve. The interface is much easier to use than the old systems—the CDC estimates it takes no more than five minutes to fill out the form and in most instances far less time than that.
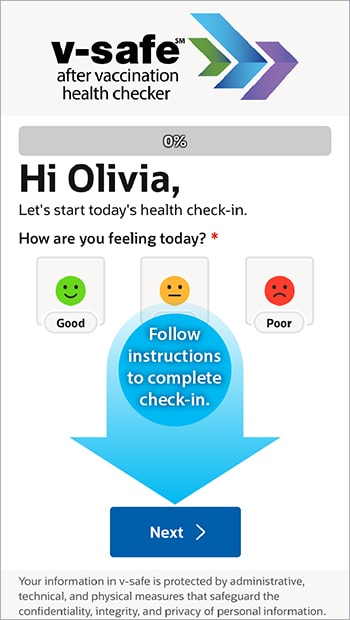
The v-safe after vaccination health checker tracks COVID-19 vaccine symptoms with personalized health check-ins.
Patient-centric insights
V-safe is more than just a weapon to help in the fight against COVID-19. It represents a new, patient-centric approach to gathering data about the efficacy of vaccines, treatments, and more.
“Access to this massive amount of real-world health data will improve the quality of decision making critical to the practice of medicine and formulation of public health policy,” says Oracle founder and CTO Larry Ellison. “We needed to get this data in the hands of researchers and medical practitioners immediately.”
Here are three ways that the approach to health data collection exemplified by v-safe has the potential to change clinical trials and healthcare.
1. Finding rare adverse reactions
Clinical trials, no matter the duration, are good at finding common adverse reactions, and not as good at finding rare reactions. They’re good at finding data in a controlled environment but not as good at uncovering data in the uncontrolled environment of post-clinical trial use of a treatment or vaccine.
“We’ve been able to rapidly collect experiences from a large population of vaccinated people that have been participating in v-safe,” says Tanya Myers, epidemiologist and team leader for v-safe at the CDC. “It's allowed us to provide information to healthcare providers that allows them to counsel their vaccine recipients about what to expect and which reactions are more common.”
2. Gaining patients’ trust
Millions of people have opted in to share their health data through v-safe, giving healthcare leaders hope that if people believe that their information is secure, and that they’re providing something that will benefit the larger community, they will take that step. “The focus going forward will be on data quality, risk management, making sure that the data being collected is correct and proper and fit for purpose for how it’s going to be used,” says Henry McNamara, senior vice president and general manager for Oracle Health Sciences. “Health systems and doctors—those are trusted partners for the population, and I think people will opt in.”
3. Improving clinical trial participation
Once people have opted in to share their data, researchers and healthcare workers can reach out to gather more data. V-safe lets participants know that the CDC may reach out to them if they report an adverse reaction. “We can ensure more citizen engagement in a couple ways—first, communicate with them as they want to be talked to, by phone, text, or email,” says Vandebelt. “Second, let them initiate the conversation.” By allowing the subject to take ownership of the interaction, Vandebelt believes that participants are less likely to drop out unexpectedly and will feel a stronger sense of commitment to the effort.
Vandebelt says that the new approaches to clinical trials and vaccine safety created by the COVID-19 pandemic have given public health and healthcare professionals hope that this will provide a new model going forward. “I think offering the community the ability to report on their symptoms or their experiences around the pandemic—that has provided them with a sense of contribution, confidence, and calm,” Vandebelt says.
Photography: Getty images